COVID-19 Perinatal Navigator
The COVID-19 Perinatal Navigator Initiative assists families experiencing pregnancy and /or with infants or very young children in navigating information and resources to sustain health and /or improve health outcomes during the pandemic.
Created in February of 2021, this community-centered program aims to ease the burden of the pandemic by providing credible information about the virus, vaccine, and policies related to COVID-19. Additionally, we are striving to connect families with critical resources and creating a good foundation for sustained health and well-being.


Community Assessment Survey
Focus Groups


VACCINE SURVEY RESULTS
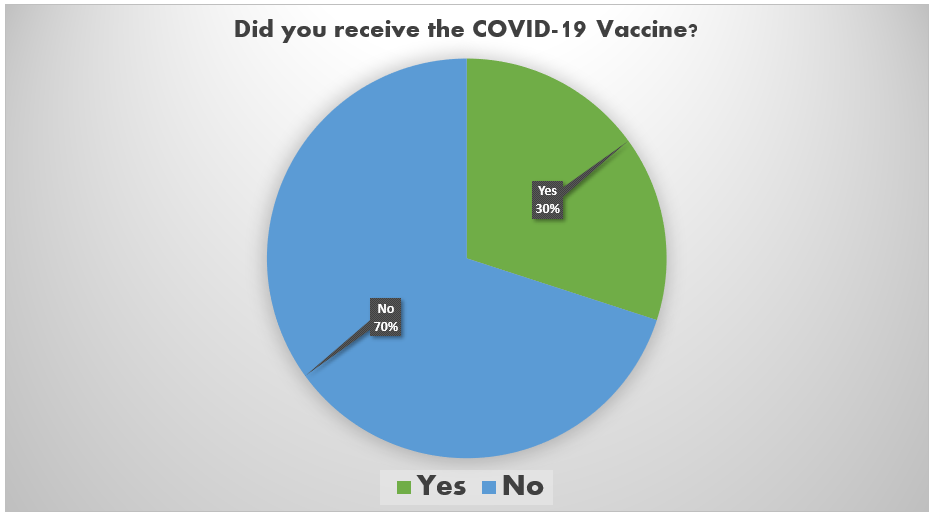
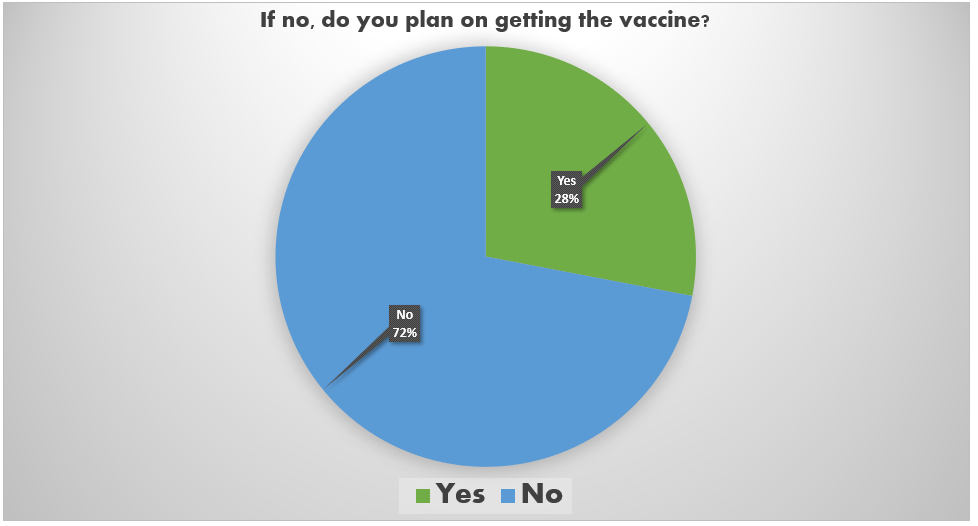
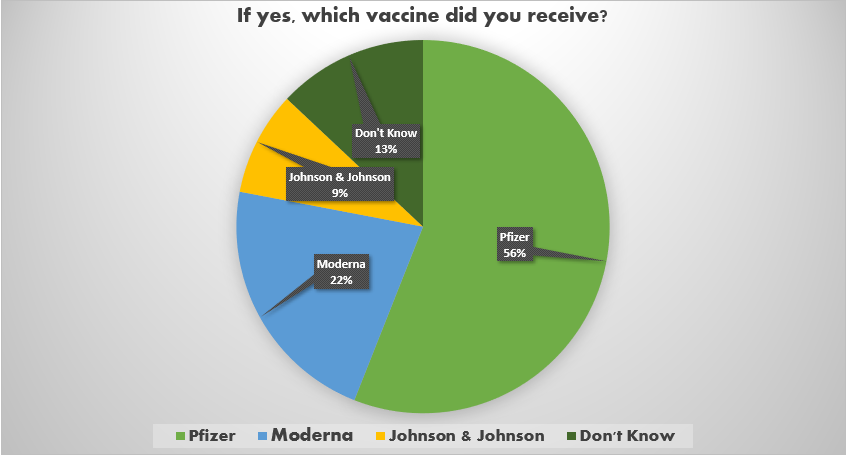
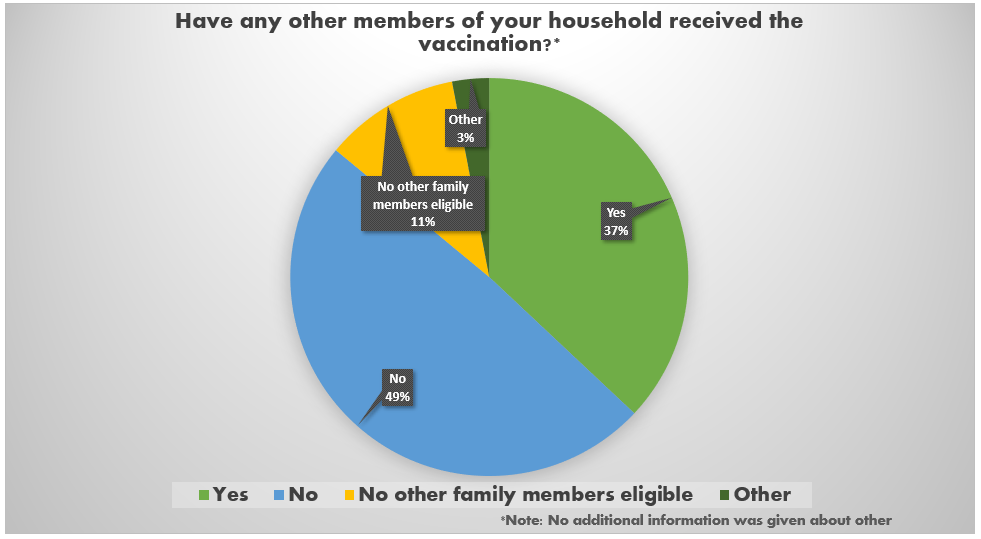
The Healthy Start COVID-19 Perinatal Navigator team is interested in how Healthy Start participants feel about the COVID-19 vaccine and community vaccination efforts. This information will help us to understand our community’s vaccine status, concerns, and issues which will inform the ways Healthy Start can provide support and services to the communities we serve.
A community survey was distributed among Healthy Start participants across all programs. In total, we received 76 responses.
Latest Updates & Resources for Allegheny County
Frequently Asked Questions
The following questions were posed by our survey respondents.
How does the vaccine affect your body?
To understand how COVID-19 vaccines work, it helps to first look at how our bodies fight illness. When germs, such as the virus that causes COVID-19, invade our bodies, they attack and multiply. This invasion, called an infection, is what causes illness. Our immune system uses several tools to fight infection. Blood contains red cells, which carry oxygen to tissues and organs, and white or immune cells, which fight infection. Different types of white blood cells fight infection in different ways:
- Macrophages are white blood cells that swallow up and digest germs and dead or dying cells. The macrophages leave behind parts of the invading germs, called “antigens”. The body identifies antigens as dangerous and stimulates antibodies to attack them.
- B-lymphocytes are defensive white blood cells. They produce antibodies that attack the pieces of the virus left behind by the macrophages.
- T-lymphocytes are another type of defensive white blood cell. They attack cells in the body that have already been infected.
The first time a person is infected with the virus that causes COVID-19, it can take several days or weeks for their body to make and use all the germ-fighting tools needed to get over the infection. After the infection, the person’s immune system remembers what it learned about how to protect the body against that disease.
The body keeps a few T-lymphocytes, called “memory cells,” that go into action quickly if the body encounters the same virus again. When the familiar antigens are detected, B-lymphocytes produce antibodies to attack them. Experts are still learning how long these memory cells protect a person against the virus that causes COVID-19.
Vaccine mechanisms:
There are two types of vaccines being distributed currently, mRNA vaccines and viral vectors.
mRNA vaccine
- First, COVID-19 mRNA vaccines are given in the upper arm muscle. Once the instructions (mRNA) are inside the muscle cells, the cells use them to make the protein piece. After the protein piece is made, the cell breaks down the instructions and gets rid of them.
- Next, the cell displays the protein piece on its surface. Our immune systems recognize that the protein doesn’t belong there and begin building an immune response and making antibodies, like what happens in natural infection against COVID-19.
At the end of the process, our bodies have learned how to protect against future infection. The benefit of mRNA vaccines, like all vaccines, is those vaccinated gain this protection without ever having to risk the serious consequences of getting sick with COVID-19.
Viral vector vaccine
- First, the vector (not the virus that causes COVID-19, but a different, harmless virus) will enter a cell in our body and then use the cell’s machinery to produce a harmless piece of the virus that causes COVID-19. This piece is known as a spike protein, and it is only found on the surface of the virus that causes COVID-19.
- Next, the cell displays the spike protein on its surface, and our immune system recognizes it doesn’t belong there. This triggers our immune system to begin producing antibodies and activating other immune cells to fight off what it thinks is an infection.
- At the end of the process, our bodies have learned how to protect us against future infection from the virus that causes COVID-19. The benefit is that we get this protection from a vaccine, without ever having to risk the serious consequences of getting sick with COVID-19. Any temporary discomfort experienced after getting the vaccine is a natural part of the process and an indication that the vaccine is working.
Do the vaccines differ?
Yes, the vaccines differ in the method of delivery and technology. The Pfizer and Moderna vaccines (two injections) are mRNA vaccines, and the Johnson & Johnson vaccine (single injection) is a viral vector. Both vaccines, however, tell the body to make spike proteins which are harmless and unique to the virus, so the antibodies the body makes recognizes the COVID virus without COVID exposure.
What will I feel like after I received the second dose? I got kind of sick after the first one.
The range of side-effects vary with each person. Some people have similar side effects to their first dose, for some people their second dose side effects may be greater than the first, and some people have only injection site soreness after the second dose.
Will you be in pain after the vaccine?
Injection site pain, redness and swelling are common after the receiving the vaccine. These symptoms should go away in a few days. Cold compresses reduce some of the discomfort. It is also recommended to use or exercise the injected arm.

Who should be getting the booster shot? CDC recommends:
- People 65 years and older and residents in long-term care settings should receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine at least 6 months after their Pfizer-BioNTech primary series
- People aged 50–64 years with underlying medical conditions should receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine at least 6 months after their Pfizer-BioNTech primary series
- People aged 18–49 years with underlying medical conditions may receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine at least 6 months after their Pfizer-BioNTech primary series, based on their individual benefits and risks
- ·People aged 18-64 years who are at increased risk for COVID-19 exposure and transmission because of occupational or institutional setting may receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine at least 6 months after their Pfizer-BioNTech primary series, based on their individual benefits and risks
Does the vaccine help protect breastfed babies?
Because the vaccines have not been studied in people who are breastfeeding, there are limited data available on the:
- Safety of COVID-19 vaccines in people who are breastfeeding
- Effects of vaccination on the breastfed baby
- Effects on milk production or excretion
COVID-19 vaccines cannot cause infection in anyone, including the mother or the baby, and the vaccines are effective at preventing COVID-19 in people who are breastfeeding. Recent reports have shown that breastfeeding people who have received mRNA COVID-19 vaccines have antibodies in their breastmilk, which could help protect their babies. More data are needed to determine what protection these antibodies may provide to the baby.
Provide more information for those of us who don’t believe it’s worth the risk.
The choice to become vaccinated is a highly personal one based on several factors. There are risks associated with vaccination and there are risks associated with catching the coronavirus. The range of symptoms of COVID-19 makes it impossible to predict the severity of the disease outcomes for each individual. While breakthrough infections (infection after full vaccination) are possible, the likelihood of illness, hospitalization and death is significantly reduced. We encourage you to make an informed decision in collaboration with your healthcare provider.
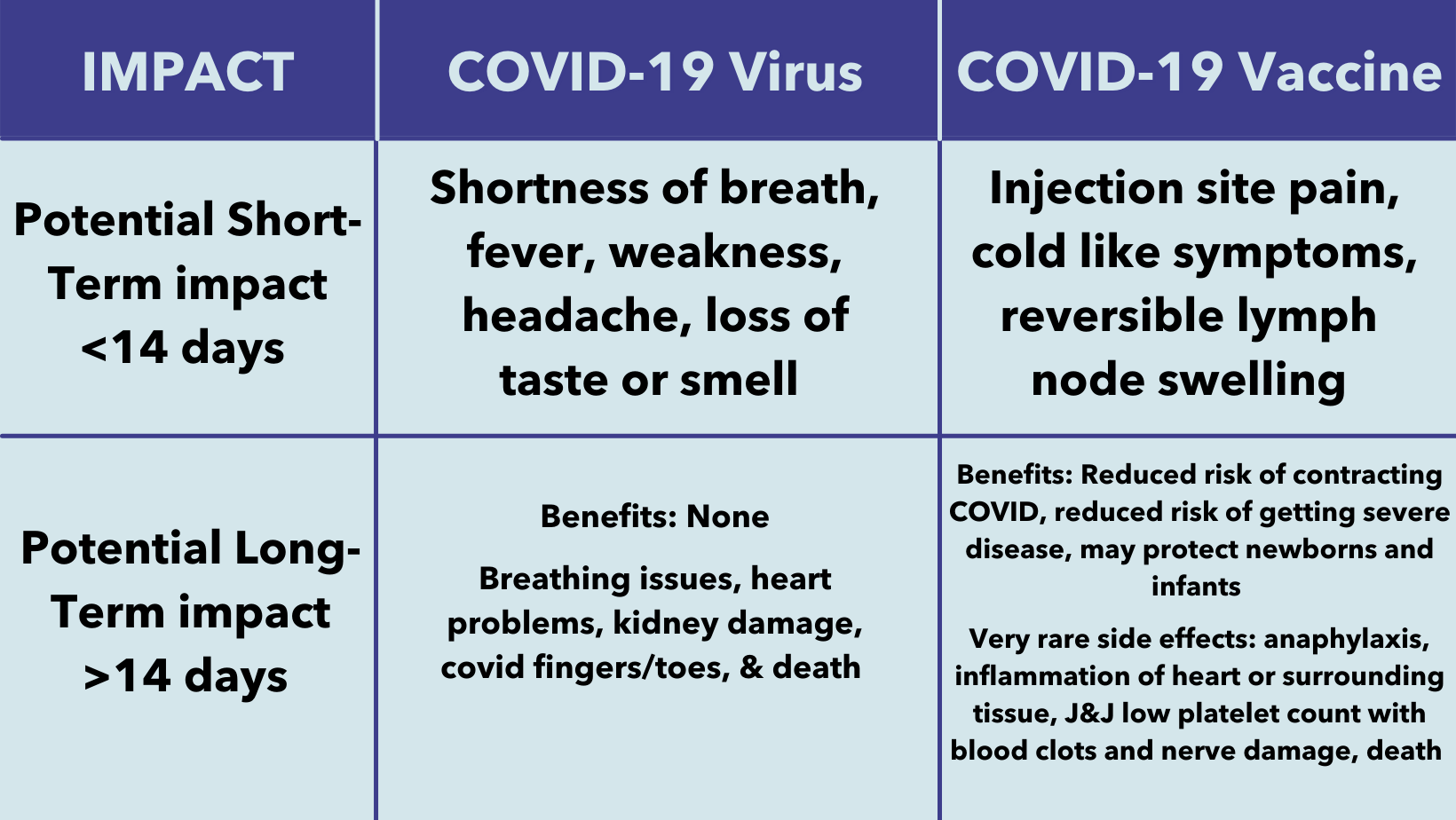
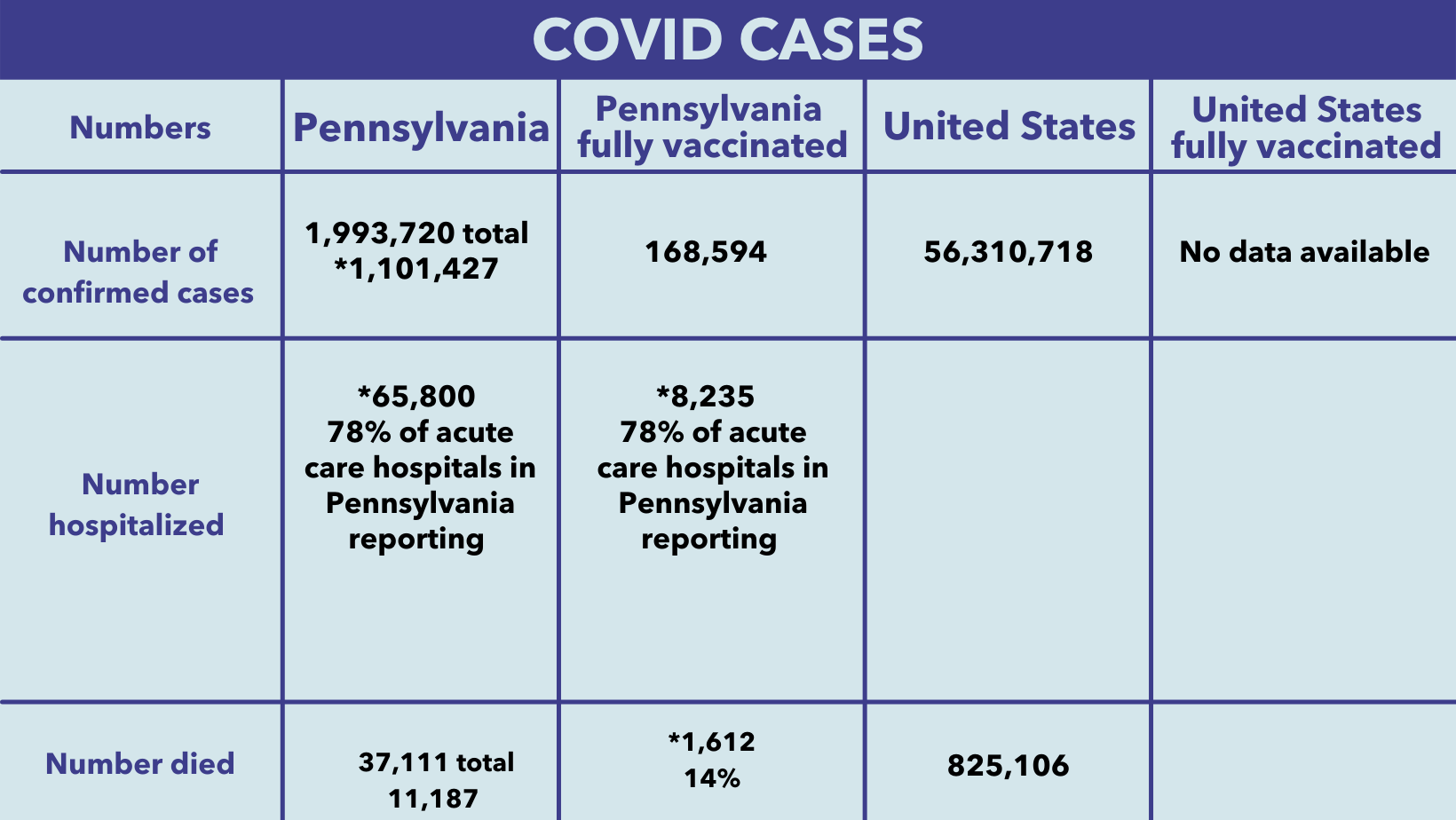
*Values reflect data from 1/1/21 to 10/4/21
**Values do not include patients who tested positive, but died from other causes, car accidents etc., as of 10/12/21
Data sources:
PA Post-Vaccination Data
https://www.health.pa.gov/topics/disease/coronavirus/Pages/Post-Vaccination-Data.aspx
COVID-19 Breakthrough Case Investigations and Reporting | CDC
Johns Hopkins Coronavirus Resource Center (jhu.edu)
COVID-19 vaccines are safe!
- While the COVID-19 vaccines were approved for emergency authorization, all steps have been taken to ensure their safety and effectiveness.
- COVID-19 vaccines were developed using science that has been around for decades.
- COVID-19 vaccines are not experimental. They went through all the required stages of clinical trials. Extensive testing and monitoring have shown that these vaccines are safe and effective.
- COVID-19 vaccines have received and continue to undergo the most intensive safety monitoring in U.S. history. Learn more about how federal partners are ensuring COVID-19 vaccines work.
COVID-19 vaccines are effective
- COVID 19-vaccines are effective. They can keep you from getting and spreading the virus that causes COVID-19. Learn more about the different COVID-19 vaccines.
- COVID-19 vaccines also help keep you from getting seriously ill even if you do get COVID-19.
- Getting vaccinated yourself may also protect people around you, particularly people at increased risk for severe illness from COVID-19.




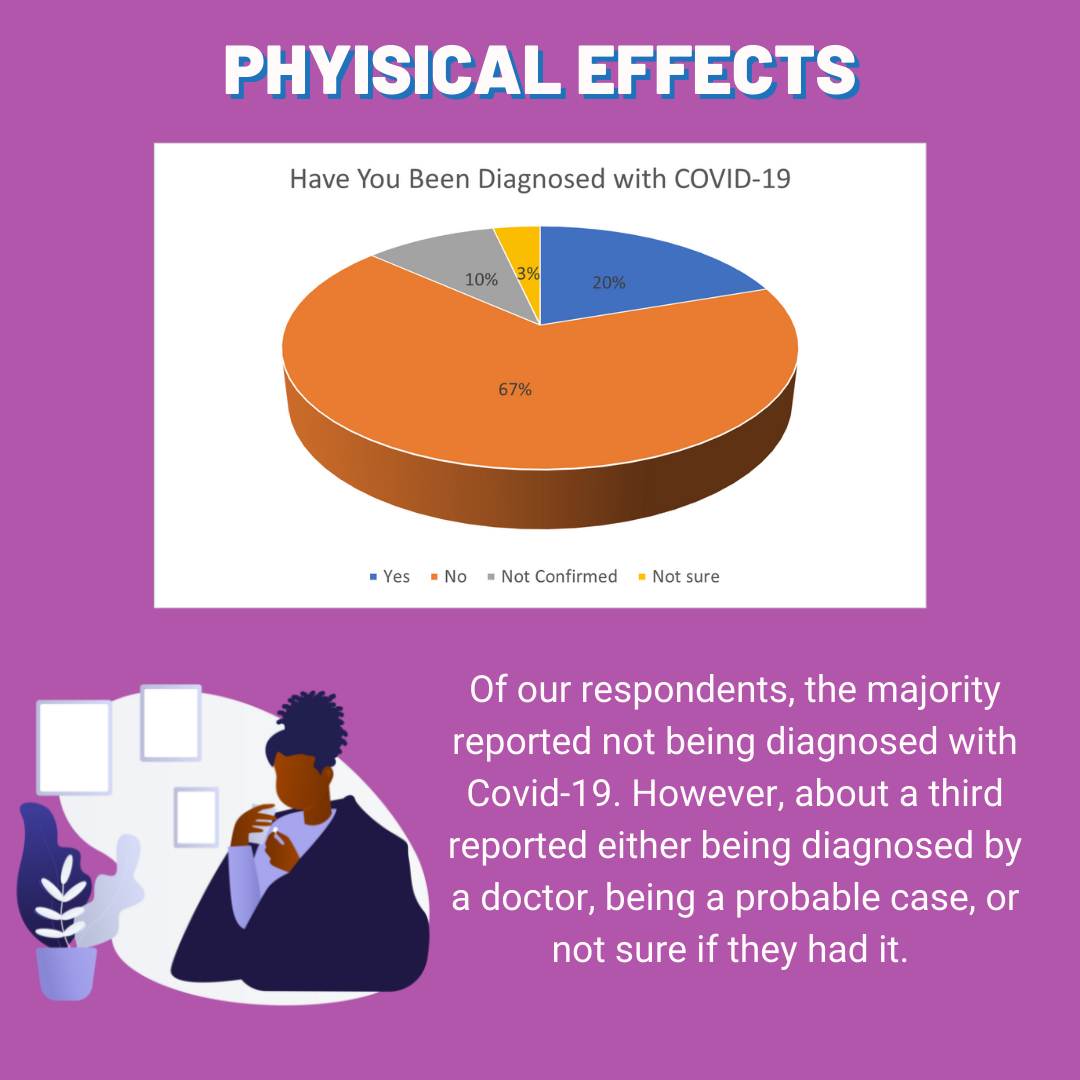


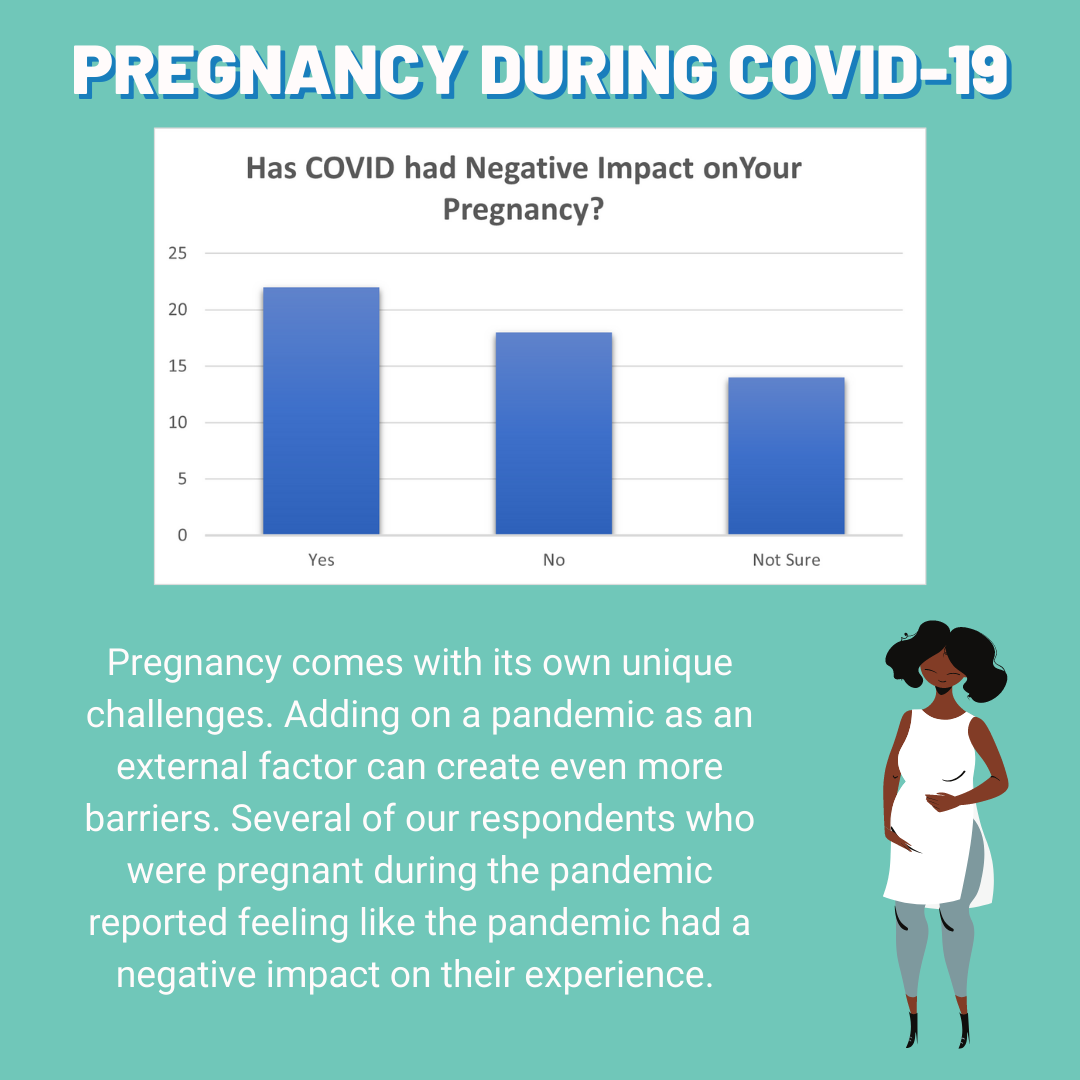
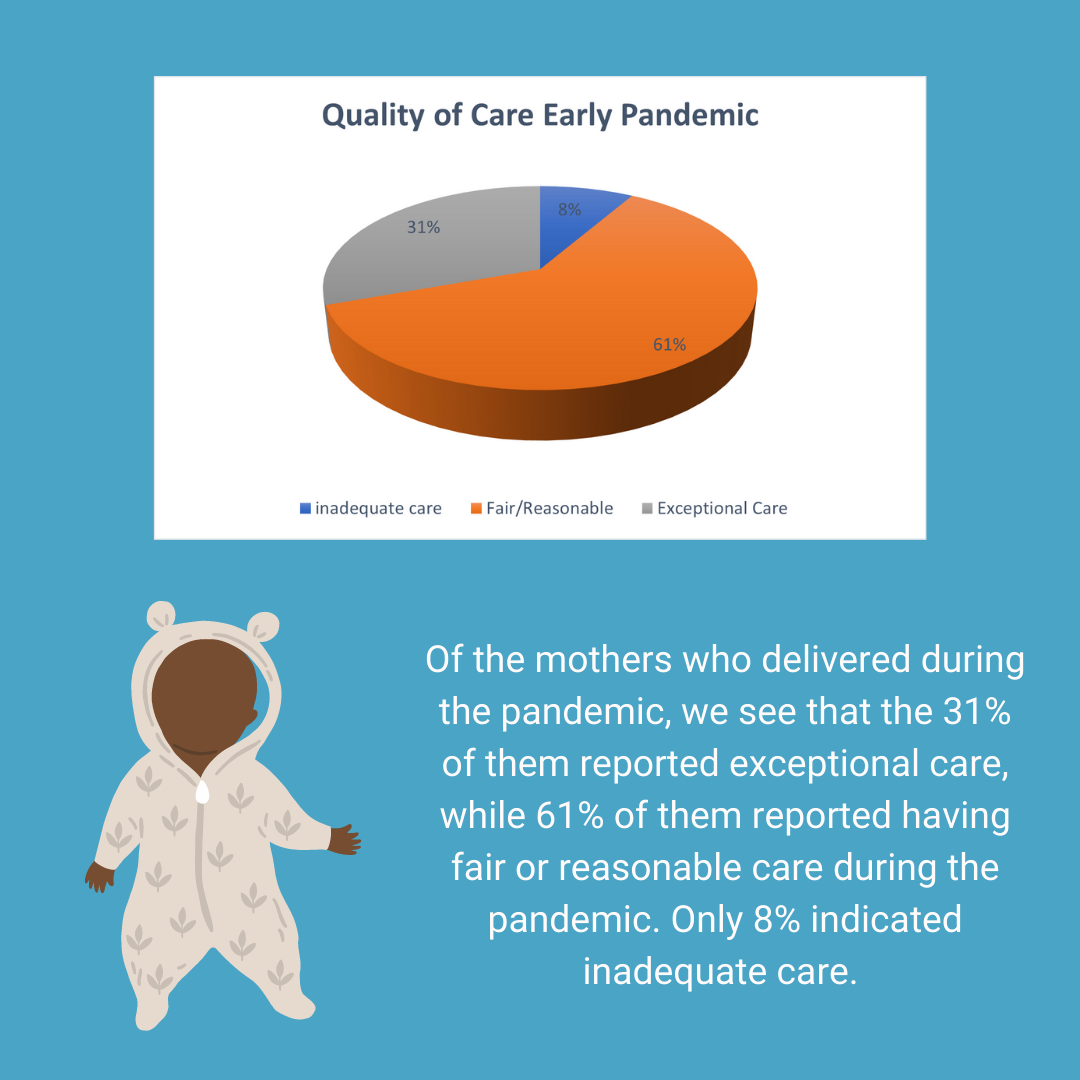
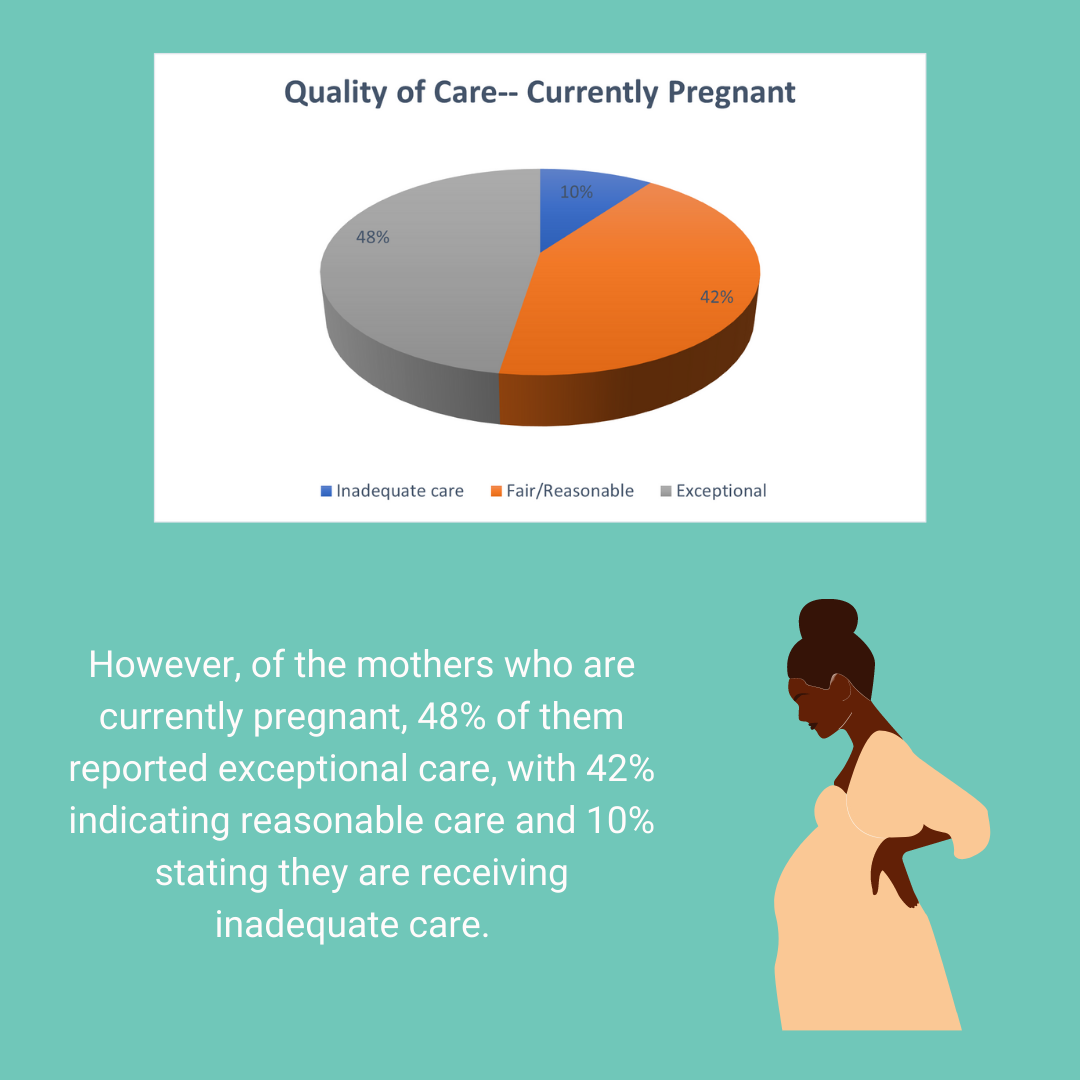

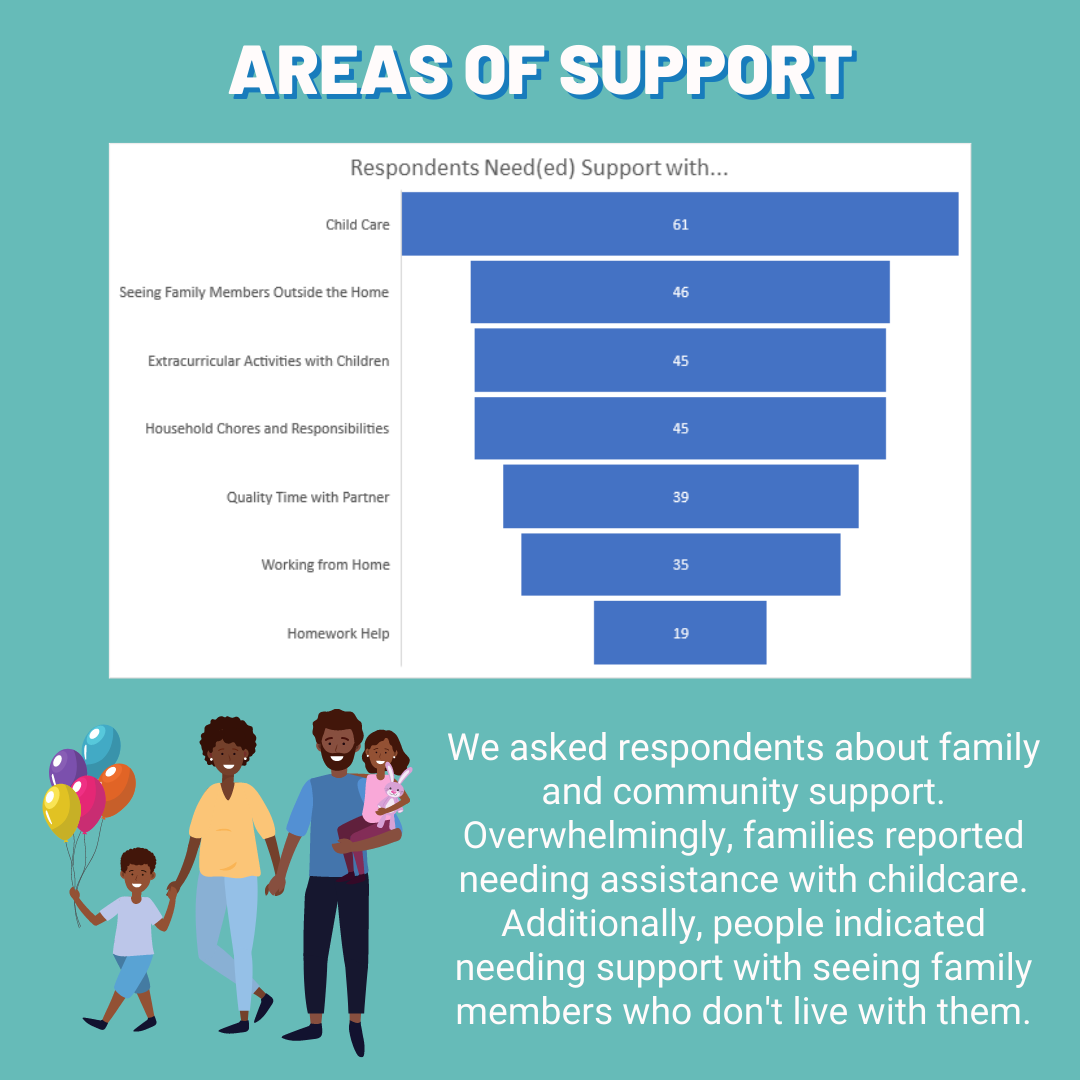











Comments are closed.